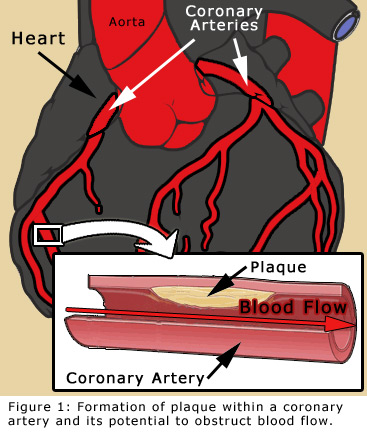
Coronary angioplasty, also known as percutaneous coronary intervention (PCI), is a procedure performed to open blockages formed from plaques in heart arteries and therefore improve blood flow to the heart. Plaques form as a result of coronary artery disease, an inflammatory process that eventually results in calcium deposits within the walls of blood vessels. If these plaques become severe enough, impairment in blood flow to the heart results.
Angioplasty procedure is commonly performed in patients who have symptoms of coronary artery disease (angina) and in patients who are actively having a heart attack. The major benefit of this procedure is to reduce symptoms (e.g. chest pain, shortness of breath) related to coronary artery disease and in some instances this procedure can reduce the incidence of myocardial infarction and death.
Angioplasty is commonly performed by placing a coronary stent (see Figure 2), a tiny pipe-like structure placed inside an artery. At locations where plaque has caused a narrowing of the blood vessel lumen, this device can return the lumen to a more normal size.
For more detailed information about the coronary stenting procedure, continue reading below.
Coronary angioplasty, if necessary, is performed following a
cardiac catheterization.
A long, thin, flexible tube, called a catheter, is typically inserted into the leg or arm through a tiny incision
(typically less than one-tenth of an inch) at the skin surface. These catheters travel through blood vessels to the heart.
A wire is then advanced through the catheter and inserted into a coronary artery.
Usually a balloon is advanced over the wire and the balloon is inflated at the location of the severe blockage or
plaque. The balloon alone can be used to treat the blockage, but in most instances, a stent is required for best
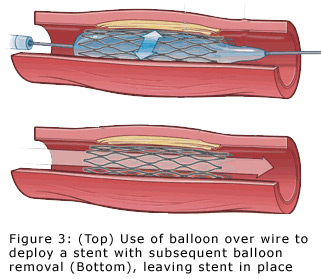
results. The stent, if needed, is initially located on the outside of a balloon. The stent and balloon are then advanced
over the wire and the balloon is inflated. The balloon inflation expands the stent up against the wall of the artery,
securing it in place. The balloon and wire are then removed, leaving the stent behind (see Figure 3 below).
 The walls of the heart artery will eventually grow around the stent, much like ivy can grow and eventually cover
a chain-link fence. While this healing process is occuring, certain medications are extremely important to take and
your physician will discuss this with you. In most instances, aspirin is required life-long, and an additional anti-platelet medication (e.g. clopidogrel, prasugrel, or ticagrelor) is needed for months to years, depending on the type of stent and reason for its
placement. Your doctor will discuss with you the specifics regarding necessary medications.
The walls of the heart artery will eventually grow around the stent, much like ivy can grow and eventually cover
a chain-link fence. While this healing process is occuring, certain medications are extremely important to take and
your physician will discuss this with you. In most instances, aspirin is required life-long, and an additional anti-platelet medication (e.g. clopidogrel, prasugrel, or ticagrelor) is needed for months to years, depending on the type of stent and reason for its
placement. Your doctor will discuss with you the specifics regarding necessary medications.
If you recently have had
a coronary angioplasty or stent procedure, and are taking medications prescribed by your physician, do not stop these medications for any
reason without consulting your doctor.



 Coronary angioplasty, also known as percutaneous coronary intervention (PCI), is a procedure performed to open blockages formed from plaques in heart arteries and therefore improve blood flow to the heart. Plaques form as a result of coronary artery disease, an inflammatory process that eventually results in calcium deposits within the walls of blood vessels. If these plaques become severe enough, impairment in blood flow to the heart results.
Coronary angioplasty, also known as percutaneous coronary intervention (PCI), is a procedure performed to open blockages formed from plaques in heart arteries and therefore improve blood flow to the heart. Plaques form as a result of coronary artery disease, an inflammatory process that eventually results in calcium deposits within the walls of blood vessels. If these plaques become severe enough, impairment in blood flow to the heart results.
 Coronary angioplasty, if necessary, is performed following a
Coronary angioplasty, if necessary, is performed following a  The walls of the heart artery will eventually grow around the stent, much like ivy can grow and eventually cover
a chain-link fence. While this healing process is occuring, certain medications are extremely important to take and
your physician will discuss this with you. In most instances, aspirin is required life-long, and an additional anti-platelet medication (e.g. clopidogrel, prasugrel, or ticagrelor) is needed for months to years, depending on the type of stent and reason for its
placement. Your doctor will discuss with you the specifics regarding necessary medications.
The walls of the heart artery will eventually grow around the stent, much like ivy can grow and eventually cover
a chain-link fence. While this healing process is occuring, certain medications are extremely important to take and
your physician will discuss this with you. In most instances, aspirin is required life-long, and an additional anti-platelet medication (e.g. clopidogrel, prasugrel, or ticagrelor) is needed for months to years, depending on the type of stent and reason for its
placement. Your doctor will discuss with you the specifics regarding necessary medications.